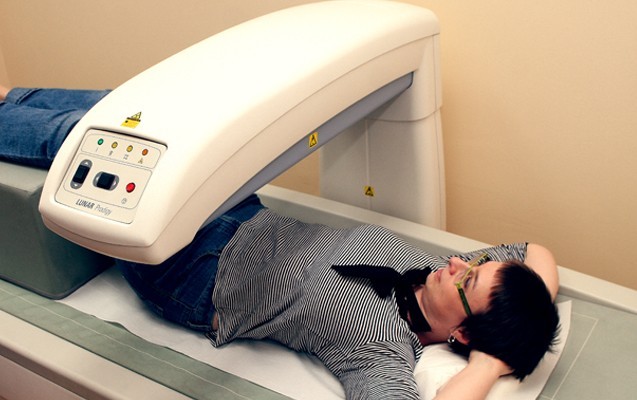
Densitometry
It is the only test that can confirm or exclude osteoporosis and assess the risk of the disease (performed on patients from 17 years old). Densitometry is painless, as is ultrasound and X-ray. The radiation dose is minimal.
Only densitometry of the spine and femoral neck allows to assess the risk of fractures and decide on treatment. Forearm and heel tests are not recommended and no diagnosis can be made from them. Spinal densitometry best evaluates early perimenopausal changes that are not visible in the femoral neck. Cervical examination assesses the risk of long bone fractures. A full densitometric examination includes the lumbar spine and the neck of the femur.
Densitometry is a basic test in the diagnosis of osteoporosis and osteopenia. It is a two-dimensional version of computed tomography. It is based on radiological evaluation of the absorption difference between the bone and fat and muscle tissue. The measurement value is expressed in two-dimensional grams (BMC – Bone Mineral Content) and in g/cm2 (BMD – Bone Mineral Density).
Densitometry can also be successfully performed in the diagnosis of atypical infections caused by CHLAMYDIA and as an auxiliary method in establishing a diet for people suffering from obesity.
The tests are performed on a high quality GE Lunar Prodigy densitometer (reference model of bone densitometer by General Electric Medical, USA). The percentage error of measurement for the densitometer we use is %CV = 0.08% (on average for older types of densitometers %CV is about 1%, the permissible error %CV=1.8% [ISCD standard]).
LSC (smallest significant change) for the densitometer we use
LSC = 2.77 * %CV, LSC = 2.77 * 0.08%, LSC = 0.002 g/cm2
[ISCD permissible error LSC = 0.050 g/cm2]
The accuracy of the device allows, if necessary, for reliable monitoring of patients at 3-month periods (important in steroid therapy patients).